Share Your Feedback on Key MFTD Waiver Updates to Strengthen Support for Families

Families have through Sept. 28, 2024, to share input on waiver amendments allowing CNAs to become paid family caregivers and nursing rate increases.
Families have an opportunity to share feedback on several significant updates to the Medicaid Home and Community-Based Services Waiver for Those Who Are Medically Fragile, Technology Dependent (MFTD waiver).
The Illinois Department of Healthcare and Family Services (HFS) is the Medicaid agency responsible for the MFTD waiver. Many families in the Home Care Program have children who receive services through this waiver.
HFS is currently seeking approval from the federal Centers for Medicare and Medicaid Services (CMS) for waiver amendments that will:
- Allow parents who are certified nursing assistants (CNAs) to be paid family caregivers
- Increase rates for in-home nurses and CNA services
Read below for more details about these amendments and how to share your input.
CNAs as Paid Family Caregivers
Plans are underway to allow parents/legally responsible adults (LRAs) to become paid caregivers if they are a CNA and employed through a nursing agency.
Currently, parents/LRAs are paid for providing skilled nursing services to their children if they hold an active registered nurse (RN) or licensed practical nurse (LPN) license. This rule applies to parents/LRAs of all children approved for Home Care services, regardless of the child’s age. (Read more about our efforts to make paid licensed family caregivers a permanent benefit.)
Allowing parents and caregivers who are CNAs to become paid caregivers is an important step in strengthening our support for families of individuals who need in-home shift nursing.
This update would give more parents/LRAs the opportunity to earn payment for the caregiving they provide their children at home.
This change requires an amendment to the MFTD waiver as well as the creation of a new state plan amendment.
Nursing Rate Increase
HFS is also proposing a 7 percent rate increase for in-home nurses and CNA services to take effect on Jan. 1, 2025.
This rate increase would affect:
- RN, LPN and CNA care
- In-home and facility-based respite care
- Nurse training rates
The proposed rates are as follows:
- RN, $57.78 per hour
- LPN, $48.15 per hour
- CNA, $32.10 per hour
We hope this rate increase can help make more high-quality nursing options available for our participant families.
Transitional Care Services provided outside the home (not an MFTD waiver service) is expected to have a rate increase from $950 to $1,300 a day. This increase would also take effect on Jan. 1, 2025.
Other Key Updates in the Amendment Include:
- Adds adaptive equipment and assistive technology as new services.
- Makes pest control a post-approval process. This change means families will not need to receive prior approval for pest control services.
- Makes the Division of Specialized Care for Children (DSCC) the entity responsible for the prior approval for home accessibility modifications, vehicle modifications, medical equipment operating expenses, adaptive equipment, placement maintenance counseling and assistive technology.
- Removes the requirement of two bids if the cost exceeds $2,000 for waiver services. This change is necessary to help increase access to services.
Share Your Feedback
The public comment period for these proposed waiver amendments is now open.
To review the full list of proposed waiver updates, you can:
- Review a hard copy at HFS’ offices at:
- 201 South Grand Ave. E.,
Springfield, IL 62763 - 401 S. Clinton
Chicago, IL 60607
- 201 South Grand Ave. E.,
The deadline to provide feedback is Sept 28, 2024.
You can share your feedback in two ways:
- Via email to HFS.HCBSWaiver@illinois.gov
- Via mail to the Illinois Department of Healthcare and Family Services, Attention: Waiver Operations Management, 201 South Grand Ave. E., 2FL, Springfield, IL 62763
This public comment process is one of the best ways you can have your voice heard.
HFS will send your comments to the federal CMS as part of the waiver approval process.
If you have questions, please contact HFS’s Waiver Operations Management Unit at (217) 524-4148 or (844) 528-8444.
Important Updates on the End of Continuous Medicaid Coverage and Appendix K

Key dates to know and an overview of the impact on DSCC participants and families
We are starting to prepare for the end of the public health emergency due to the COVID-19 pandemic. We’ve put together important information about how it will affect our Division of Specialized Care for Children (DSCC) participants and their families.
When the public health emergency took effect in 2020, the federal government allowed continuous Medicaid coverage and flexibilities for individuals receiving services through a Medicaid waiver. The federal government has signaled that the public health emergency will end on May 11, 2023. Please note the federal Centers for Medicare and Medicaid has not yet confirmed this date in writing.
We want to keep our participants as up-to-date as possible and will let you know if this date changes. In the meantime, we want to explain what changes will occur once the public health emergency and continuous Medicaid enrollment end.
The following sections give an overview of:
- The end of continuous Medicaid coverage
- The changes for all DSCC participants and families
- The impact on those enrolled in the Home Care Program
End of Continuous Medicaid Coverage
When the public health emergency began in 2020, the federal government allowed for continuous Medicaid coverage. This flexibility meant no one would lose Medicaid coverage during this time. The federal government is now ending continuous Medicaid coverage on March 31, 2023.
Starting April 1, Illinois Medicaid must review eligibility for all Medicaid cases. This process is called redetermination. Redetermination is when Medicaid looks to see if you are still eligible. They look at your residency, monthly income and other criteria to decide if you still qualify.
Medicaid will send forms to some members as early as May 2023. They will not complete redetermination on all cases at the same time. They will make the redeterminations over several months. This means that your Medicaid redetermination could happen in May or later this year.
It is important to make sure Medicaid has your current address. You can report your address online at Medicaid.illinois.gov or call (877) 805-5312. We also have a news post with more details about how to update your address. Please watch your mail for letters from Medicaid.
Once you receive your redetermination notice, you will have about a month to respond. Medicaid may ask for more information about your income, residency, or other information. If Medicaid asks for more information and you do not respond, your Medicaid coverage ends. You can return the redetermination in several ways:
- Online at ABE.illinois.gov using Manage My Case. Manage My Case is the quickest way to complete your redetermination.
- By mail.
- In person at a local Illinois Department of Human Services (DHS) Family Community Resource Center.
- By phone.
If you are in a Medicaid managed care plan (MCO), please remember the MCO does not do the redetermination. Medicaid does redetermination reviews. If you do not qualify for Medicaid anymore, your coverage ends. If you are still eligible, you keep your Medicaid coverage.
Don’t risk losing your health insurance. Please update your address with Illinois Medicaid. It’s easy, fast and free:
- Call (877) 805-5312 from 7:45 a.m. to 4:30 p.m., Monday through Friday.
- Visit medicaid.illinois.gov.
- If you use a TTY, call (877) 204-1012.
Please contact your DSCC Care Coordinator if you have questions about Medicaid redetermination.
Changes for All DSCC Program Participants:
- In-Person Visits: The public health emergency has allowed flexibility for in-person visits. As the public health emergency ends, DSCC must resume all in-person visits by Nov. 11, 2023. Your DSCC Care Coordinator will work with you to schedule your next in-person/home visit.
- Verbal Signatures: The public health emergency also allowed your Care Coordinator to receive necessary signatures verbally. As the public health emergency ends, we can no longer accept verbal signatures beginning May 11, 2023.
Impact on DSCC Participants in the Home Care Program:
The COVID-19 public health emergency has allowed several flexibilities for those in the Home Care Program in two separate areas:
- Continuous Medicaid and program enrollment for those found ineligible for services beginning March 1, 2020
- Appendix K flexibilities (Appendix K is an emergency coverage document for individuals receiving services through a Medicaid waiver.)
The following is important information about how the end of the public health emergency will affect Home Care Program participants.
End of Continued Medicaid and Program Enrollment for Those Found Ineligible for Services:
- There have been no reductions or loss of eligibility for Home Care participants since March 1, 2020. In 2022, the federal government separated the continuous Medicaid enrollment coverage provision from the public health emergency. As a result, continuous Medicaid coverage will end on March 31, 2023.
Starting April 1, 2023, DSCC will work with the Illinois Department of Healthcare and Family Services (HFS) to determine eligibility. We will reassess all Home Care Program participants who received a notice of ineligibility for the program since March 1, 2020. If you or your child received a notice of ineligibility for services since then, your services will remain in place until we complete a reassessment. The reassessment will look at your updated and current medical documentation. This includes individuals who appealed and were still deemed ineligible for services. Based on the new reassessment, HFS will send you an updated notice. This notice will state whether you or your child are eligible for Home Care services. Your DSCC Care Coordinator will work with you to complete a reassessment before Sept. 30, 2023.
- If you or your child received a notice of reduced nursing hours since March 1, 2020, your Care Coordinator will complete the next reassessment of services at your regularly scheduled renewal time. Services will remain in place until this reassessment occurs. After this reassessment, HFS will send you a new notice based on updated and current medical documentation. The notice will list the new level of services.
More Information for Individuals in the Non-Waiver Program (Nursing and Personal Care Services):
- You will no longer receive Home Care Program nursing services if you or your child turned 21 and are not on the MFTD waiver but still receive nursing. Your nursing services will end on Sept. 30, 2023. Your Care Coordinator will work with you to ensure you, or your child is set with an alternate state waiver, such as the Division of Rehabilitation Services (DRS), if applicable. If you or your child will turn 21 on or after March 31, 2023, services will end on the date indicated on the current notice of ineligibility.
- For all non-waiver participants under age 21, you must continue to have Medicaid coverage to receive Home Care services. It is important that you submit the redetermination form from Medicaid to keep your coverage. If you fail to meet Medicaid eligibility or do not respond in time, HFS will cancel your Medicaid case. Your Home Care services will then also end. For more information on the Medicaid redetermination timeline, see the dates above.
Appendix K Flexibilities
Appendix K is an emergency coverage document for individuals receiving services through a Medicaid waiver. Appendix K provisions took effect on March 1, 2020, to give flexibility to Home Care participants. Appendix K is tied to the public health emergency, which is determined by the federal government.
As we noted above, the federal government has indicated the public health emergency will end on May 11, 2023. Appendix K provisions would then continue for six months after the public health emergency ends. Therefore, Appendix K flexibilities will end on Nov. 11, 2023. However, DSCC worked with HFS to make two flexibilities permanent. Here are more details on what will change and what will remain in place:
- Licensed (RN or LPN) parent/LRA paid caregivers: Parents/legally responsible adults (LRAs), including foster parents, can continue to provide skilled nursing services to their child if they hold an active registered nurse (RN) or licensed practical nurse (LPN) license. DSCC sent a separate notice on this provision remaining permanent, which includes details on guidelines. (You can also read our news post on Home Care Program Changes Give Families More Flexibility and Support.)
- Overtime: Nursing agencies will permanently receive payment for providing overtime hours to Home Care participants. DSCC sent a separate notice on this provision remaining permanent, which includes details on guidelines. (You ou can also read our news post on Home Care Program Changes Give Families More Flexibility and Support.)
- Additional COVID-19 respite allotment: During the public health emergency, HFS approved an additional 336 hours of respite to use before the regular respite allotment. This additional respite is for all Home Care MFTD waiver participants. Starting Nov. 11, 2023, this additional COVID respite will expire. All respite used after Nov. 11, 2023, will come from the standard respite allotment.
- Personal Protective Equipment (PPE): During the public health emergency, nursing agencies were reimbursed for PPE when actively staffing nurses in the home. The PPE is for the nurses to use while caring for participants. This reimbursement of PPE supplies to the nursing agencies will end on Nov. 11, 2023.
- Nursing Supervisory Visits: Nursing agencies resumed in-person supervisory visits in November 2020. Effective May 11, 2023, there will be no exceptions allowed to replace in-person supervisory visits.
Please contact your DSCC Care Coordinator at (800) 322-3722 if you have questions or are unsure how this information may impact your family.
We are thankful for your partnership throughout the pandemic and public health emergency. Our team will continue to help support your family and connect you with the right services and resources.
Permanent Home Care Program Changes Give Families More Flexibility and Support
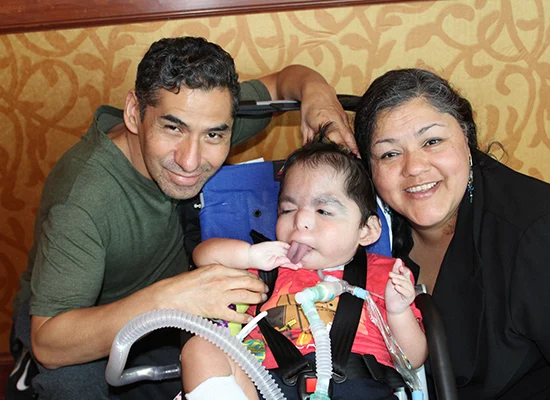
Paid licensed caregivers and nurse overtime are now permanent options for Home Care families
We have exciting news about long-term changes to the Home Care Program. We have listened to our participant families and made two pandemic-related benefits permanent. These changes can provide continued flexibility and support beyond the public health emergency.
When the COVID-19 pandemic began in March 2020, UIC’s Division of Specialized Care for Children (DSCC) partnered with the Illinois Department of Healthcare and Family Services (HFS) to address our Home Care families’ needs. Together, we set provisions included in Appendix K. Appendix K is an emergency coverage document for individuals receiving services through a Medicaid waiver.
We continued to partner with HFS to make two provisions permanent for Home Care participants. As a result, nurses can continue to provide overtime. Licensed parents/legally responsible adults (LRAs) can also remain paid nurse caregivers for their children enrolled in Home Care.
Below are more information and guidelines on these new permanent changes.
Licensed (RN or LPN) Parent/LRA Paid Caregivers
Parents or LRAs, including foster parents, can provide skilled nursing services to their children if they hold an active registered nurse (RN) or licensed practical nurse (LPN) license.
This approval includes participants enrolled in medically fragile, technology-dependent (MFTD) waiver services and non-waiver services. This approval is for all children approved for Home Care services, regardless of the child’s age.
Guidelines include:
- The licensed parent/LRA must be a nurse employee of a DSCC-approved nursing agency. The nursing agency sets the number of hours the parent can work each week.
- Services may begin on the licensed parent/LRA’s hire date.
- The licensed parent/LRA must meet all nursing agency rules for provider qualifications and training.
- The licensed parent/LRA can work overtime hours. Overtime is anything over 40 hours a week.
- The licensed parent/LRA must hold an active RN or LPN license.
- Licensed parents/LRAs may not provide respite services under the waiver.
- Licensed parents/LRAs cannot receive reimbursement for nurse training.
- The total nursing hours may not exceed the approved resource allocation.
Overtime
Nursing agencies will permanently receive payment for overtime hours to Home Care participants. Overtime hours benefit the participant and family. They also allow nurse caregivers to provide more nursing coverage to participants. The possibility of overtime also incentivizes the nurse caregiver to provide more coverage. Overtime allows nursing agencies to cover more authorized hours while stretching their staffing over fewer nurses. This is especially helpful to families during a time of increased demand for nurses.
Guidelines include:
- Under the Fair Labor Standards Act, overtime is anything over 40 hours a week.
- The Nurse Practice Act prohibits working more than 16 hours in a 24-hour period. An eight-hour break between shifts is also mandatory.
- Overtime is defined as time-and-a-half.
- Overtime reimbursement comes from the approved resource allocation. The amount billed cannot exceed the HFS-approved resource allocation.
- Those on the MFTD waiver cannot use overtime when using respite hours.
- Parents/LRAs who are nurse paid caregivers can work overtime. The parent/LRA is an employee of the nursing agency. The nursing agency determines the number of hours the parent can work each week. The number of hours cannot exceed the approved resource allocation.
- Nurses can only be eligible for overtime when Medicaid is the payer. When private insurance is the payer, nurses cannot receive overtime pay.
Please contact your DSCC Care Coordinator with any questions or concerns.
We hope these permanent changes will continue to benefit your family.


